It’s now been more than two years since many workers were sent home, and while the pandemic is easing, some just aren’t coming back to the office. This blog looks at what this means for hiring and retention as many employees regard working from home as worth anything from a 5-10% pay raise!
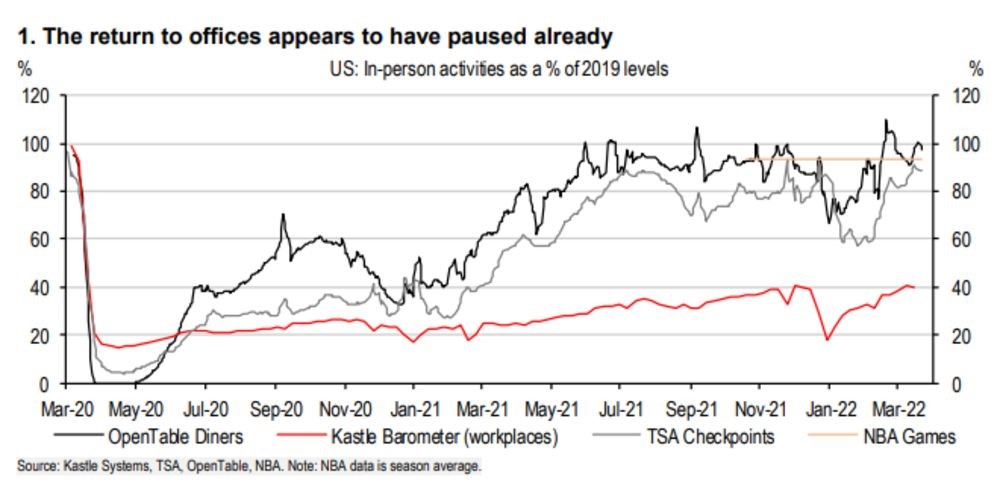
In a new report, HSBC economist James Pomeroy noted office attendance rates are struggling to get back above 40% to 50% of where they were before the coronavirus hit. Data from Kastle Systems for the U.S. shows the current highest rate of office occupancy is Austin, Texas, and that’s still only 53%. The lowest is San Francisco at around 30%.
And it’s not just the US. As of February, Transport for London data recorded only 70% of 2019’s journey volumes, suggesting commuting is still down.
Employer HR now faces a new competitive issue when it comes to hiring and retention. What is your working from home or hybrid working policy going to be? How will it impact organizational effectiveness? How will it help attract new talent and retain existing talent? This could be “forever”.
That’s all despite restaurants, cinemas and flights seeing as much as 90% of the 2019 volumes, which implies people are confident going out — just not to the office.
“With offices only half full in most of the developed world, many will be expecting office occupancy to grind higher,” said Pomeroy. “However, it’s worth keeping in mind the alternative: that occupancy could already be close to a peak.” This could be forever.
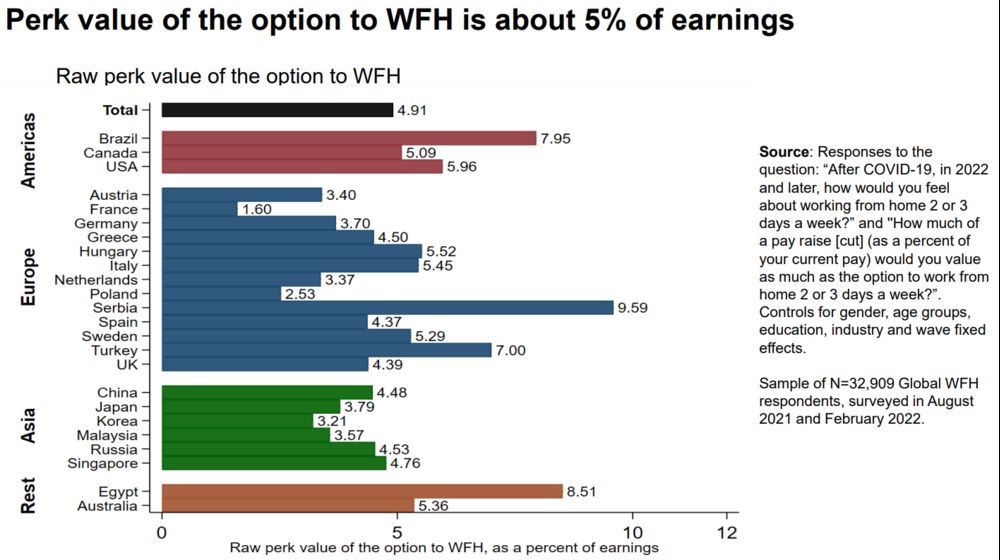
The trend is evident in other data. WFH Research reported earlier this month that according to its survey of more than 32,000 people in 25 economies, the average worker values a day from home as much as a 5% pay rise.
Serbians associate flexibility with 10% more pay, while Americans reckon it’s worth a 6% hike.
Furthermore, 15% would seek out a new job if their current employer forced them back to the office five days a week. The numbers are higher in the U.K., Australia and Canada.
This is not surprising. Employees faced with the prospect of going into New York City regularly sited additional costs of up to $10,000 a year in travel costs (Vehicle depreciation, mileage, public transportation, lunch, additional dry cleaning, etc.) plus lost personal time.
An employee driving 20 miles a day to work is spending 10,000 miles, or around $5,000 a year, in after-tax income just to get to work and back.
There’s also a gap between the hopes of workers and employers. WFH Research’s survey indicates employee’s desire about two working days at home each week. Bosses are generally planning offering just one even though the same study suggests staff are 4% more efficient when at home versus business premises.
Pomeroy sees various economic implications from the latest data:
- Businesses will need to compete in different ways to attract talent, be it by offering a hybrid experience or more flexible hours.
- Rent and house prices are now being driven by demand for suburban and rural properties rather than homes in city centers. Many employees have, or want to, relocate to lower cost areas.
What does this mean for hiring and retention?
- If you have positions that could be done from home, or are being done from home, make sure the working from home option is a big part of your job postings.
- If retention is a concern, develop a hybrid working plan so existing employees can take advantage of working from home if they want to.
- Working from home is not for everyone or every organization. Make sure your hybrid working plan addresses the needs of all types of employees, including those who enjoy coming into the office.
- Establish clear rules for working from home and regular remote meetings. Consider mandatory video calls.
- Employees still want to socialize with colleagues. Consider taking savings in rent from the reduction in leases/square footage. Use that money to fund team building events.
- Consider paying employees who work from home a non-taxable stipend for using their mobile phone.
- Some companies allow extra flexibility for employees with young children to manage disrupted day care and school schedules.